Lab Technologies
By providing early and accurate results, our goal is to minimize doubt and maximize the confidence our customers and their patients have in their decisions and diagnoses.

Tests
A world-class menu of assays with more in the pipeline.
Cytology
Leading the charge in cervical disease prevention.
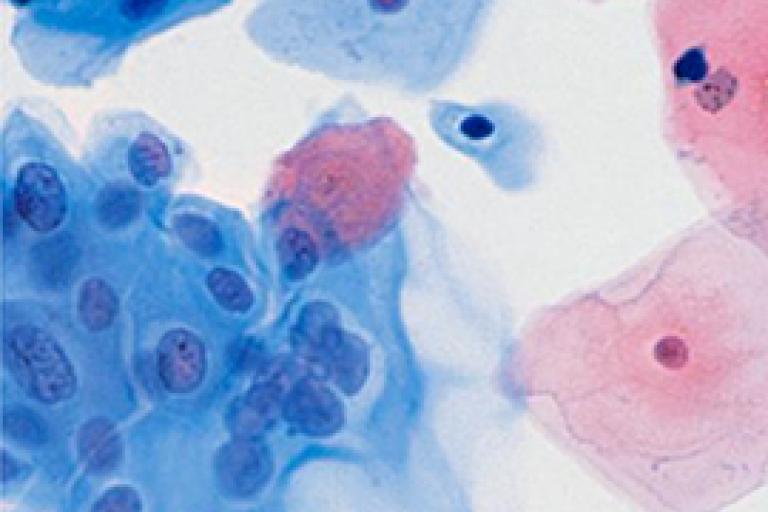
Screening Technologies
Improve your odds of detection and streamline your workflow.
Molecular Diagnostics
Automated equipment and a menu of tests that meet your needs today and tomorrow.

Collection Devices
Rigorously developed for highly accurate and reliable results.